May is pelvic health awareness month and I am supporting initiatives to help raise awareness through a series of interviews with women who are living with interstitial cystitis and other chronic pelvic pain conditions.
This interview is with Zoe, who I connected with on my Instagram and has been so kind and an amazing support for me with all the 'bladder things' that I have gone through. Zoe is a leading patient advocate in the chronic illness community and, as a qualified physiotherapist, personal trainer and Pilates instructor, provides really informative resources that help others add movement and exercise into their lives. I'm sure you will find her story inspiring and very helpful.

Can we begin with you telling us about how you came to be diagnosed with IC/ BPS? Had you lived with symptoms for a long time before your diagnosis?
As a child I would regularly get bladder infections which continued throughout my teens. In my early 20’s I started to get episodes of feeling like I was unable to fully empty my bladder. I would get my urine tested but it would come back normal, yet I’d feel constantly desperate for the loo. I had a back injury in 2016 which made these episodes worse but still didn’t do anything about it. In 2017 I became acutely unwell and needed surgery. I woke up from the operation and couldn’t empty my bladder. Eventually I did but still felt desperate constantly. I had repeated bladder infections and then the pain just never dropped back down again.
My GP referred me to a numerous specialists until eventually a rheumatologist diagnosed me with lupus. However, my bladder issues continued to be awful and I ended up in A&E numerous times. I had really poor treatment on numerous occasions – they didn’t even scan my bladder and offered me paracetamol! After numerous cystoscopy’s and urodynamics testing I was diagnosed. I was put under the umbrella of bladder pain syndrome, but the pain and inflammation I have is due to my bladder being unable to empty due to an issue with urethral sphincter (Fowlers Syndrome). It is unable to release urine, so I end up in retention, which causes infections and keeps the cycle of pain and inflammation continuing.
How do you manage your condition? Are medications and bladder instillations helpful? Are there any lifestyle measures that help you?
I now use a supra pubic catheter (SPC) which I couldn’t live without, but it also causes numerous issues. My bladder is constantly spasming as it doesn’t like having something in it, and then my urethra joins in too. I take numerous anti-spasmatic medications and pain killers to help manage this. I am on continuous antibiotics to prevent infections and have a bladder instillation which also helps to calm my bladder lining and protect from infections.
I do relaxation work and self-release techniques on my pelvic floor as the pain in my bladder makes it spasm. I also use numerous breathing techniques and stretches to help combat the effect of a painful bladder on my body.
You have been very open about the issues you have had using catheters, and now have a suprapubic catheter. Can you explain a little about how yourself and your doctors came to this decision for your care?
It was during urodynamics that they realised I could not pee. They filled my bladder up and then I was unable to release any urine so they said I would have to use a catheter to empty. I self-catheterised for a year, and managed for 6 months with an indwelling catheter but my urethra would stop these from emptying, acting like a clamp around the tube. The spasms would be so strong it would stop urine from draining and I would end back in the cycle of retention, infections and more inflammation and pain.
I had my supra pubic catheter put in July 2019 which is amazing as it bypasses my urethra so it works a lot better than the other options.
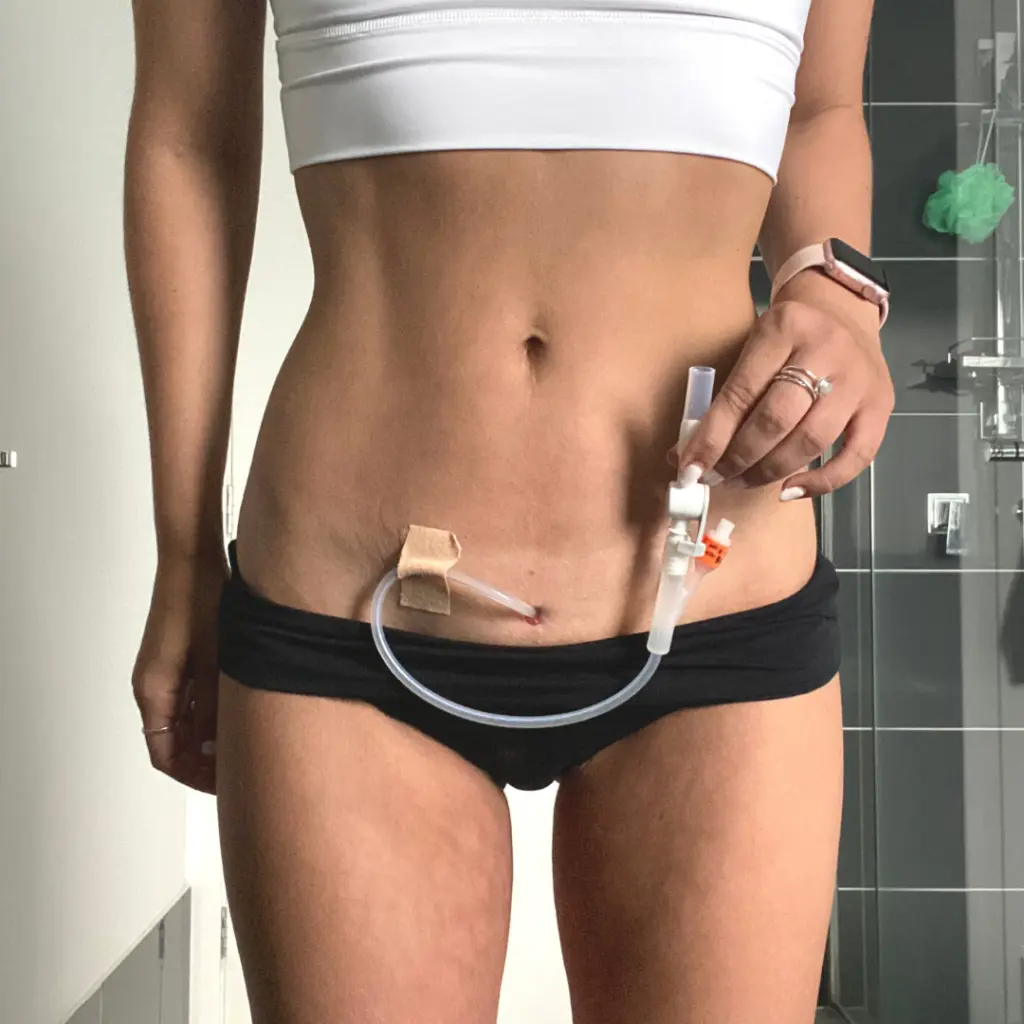
Does having a SPC limit your daily life? Or has it enabled you to do more?
My SPC has given me back my life. When I had no catheter I was in agony with constant infections, then self-catheterising helped drain but I had to catheterise so often and it was so painful that I would be up until 2-3am every night crying in the bathroom with a full bladder desperate to empty so I could try to sleep. With the urethral catheter I could not walk or sit down without it causing crazy spasms and pain.
With my SPC on a good day I barely notice it’s there. I can exercise, I can walk, I can sleep. However changes are painful and it takes my body a few weeks after a change to settle. When my bladder spasms it really stops you from doing anything. If I put an ice pack between my legs, hot water bottle on my stomach, take my meds and lie completely still, the spasms are tolerable.
Exercise is a big part of your life, and you share brilliant low intensity exercises on your Instagram and website. Do you feel that exercise is beneficial for you in terms of symptoms?
Exercise is hugely beneficial, and I generally feel worse when I don’t exercise. It’s frustrating when my bladder pain is so high that I can’t always exercise, but I still manage to find some way of moving even it is deep breathing or upper body exercises. The weaker you are, the harder everything is to do. Pain has an inhibitory effect on our muscles, so it’s important when you have pain to do what you can to maintain your strength.
It’s also important to understand the effect your pain and symptoms has on the rest of the body. I work on both strengthening and relaxing my pelvic floor muscles, as well as stretching the muscles around the pelvis to help combat the effects of constant pelvic pain.
What advice would you give to someone who wants to start to exercise, but lives with IC or other chronic illness?
Be kind to yourself – I feel like we all have so much to deal with anyway, with pain and our symptoms, plus all the medical stuff we have to carry. I strongly feel exercise should be done in a compassionate way, treat it as self-care. Find something you enjoy and feel you can do and start really slowly, building up bit by bit once you know what you are doing isn’t increasing your pain or symptoms.
With bladder pain it’s about finding what you can do that feels comfortable. Pelvic stretches are useful to incorporate into your routine. Plus strengthening the muscles in your core and around your pelvis are just as important to provide support. If you are new to exercise I recommend you seek guidance from a physio/physical therapist with experience with pelvic pain.

What are your hopes for the future with your pelvic health condition? Are there any treatments or lifestyle measures you hope to try?
My motto is ‘least intervention possible’. I feel with my body and in particular my EDS (Ehlers-Danlos syndrome), it doesn’t like intervention. Any procedure or surgery has a huge impact on my body so I try to minimise that. I only have what I really need and what my doctors advise. In saying that I also want to function, I want to be able to walk and sit at my desk, to see friends and not be stuck in the loos, to try to be able to sleep at night. Whatever options can let me do that I will consider.
I think all bladder stuff sucks. Tests and treatments are all invasive, and at the moment all the future options just sound like a lot more intervention with no promise of increased function for me. However, over the years I have filled my bladder pain ‘toolbox’ with so many things that I now feel I understand my bladder and feel more in control of what I can do to help. I feel as a community of people with bladder pain, we are learning together and I hope that soon research will catch up with us. I hope we will be met with more knowledge and understanding of the struggles of having bladder problems and not just told to take some paracetamol.
Thank you to Zoe for contributing her story to this series of interviews for pelvic health awareness month. You can find Zoe on her Instagram @activelyautoimmune and her website activelyautoimmune.com.
Please follow the advice of your doctor as to all medical treatments, supplements and dietary choices, as set out in my disclaimer. I am not a medical professional, and this post, as well as all other posts on this blog, are for informational purposes only.







Rob Hopwood says
I've suffered with weak bladder / neurogenic bladder for nearly a decade.
I tried using the valve you have for 18 months until December 2020. It made life much easier and less painful, but I got continual infections from it whatever method I used. I ended up having to drink too much water, and then couldn't sleep.
So I've had to go back to a bag on my lower leg. Because the bladder is empty most of the time, exercise causes inflammation and pain pretty quickly. And having the weight on the left leg led to an injury of the right hip in the first month, so now I can't even change the leg the bag is on! In the meantime, my leg muscles are wasting away, and I'm in pain every day. I've had to resort to psychiatric medications for now, although I didn't want to do so. Seem to be stuck in a catch-22 situation, as these bladder problems often are.
throughthefibrofog says
So sorry to hear that you are having such difficulties. I think Zoe, who I interviewed for this post, has had repeated infections as well. She now has a suprapubic catheter, which comes with its own issues. Perhaps a referral to a physiotherapist may be helpful if you haven't tried it before? They may be able to give you some exercises that don't trouble the bladder and cause further issues. Wishing you the best going forward.